Damage to Articular Joint Surface – Cartilage Preservation
Cartilage preservation is your best bet for protecting the health and performance of joints. Cartilage acts as a buffer against joints grating against each other. Treatments can aid in significantly reducing pain and go a long way towards restoring proper function.
Causes
Acute:
Injury / Trauma (eg Sporting Injuries)
Chronic:
- Degenerative Joint conditions (Osteoarthritis)
- Inflammatory Joint diseases
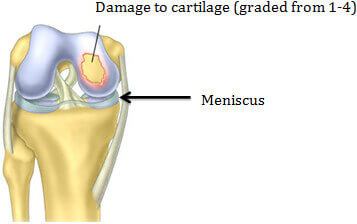
Symptoms of Damaged Articular Cartilage:
- Pain and Discomfort
- Swelling – could be intermittent with the pain
Diagnosis of articular cartilage damage:
A specialist orthopaedic surgeon will thoroughly examine the joint and gain a clear picture of a patient’s clinical history before making a recommendation on treatment.
Investigations (Tests):
- Xrays: Only show bone and joint abnormalities. These are important to make sure there is no structural damage that could inhibit cartilage preservation.
- MRI scan: Diagnoses joint surface and meniscal problems. Most patients will have an MRI scan before any procedure on the knee joint.
What non-surgical options are available for remedying damage and effective cartilage preservation?
- Activity modification and/or bracing
- Weight loss and exercise
- Cease sporting activities
- Pain relief medications such as NSAIDs
- Viscosupplementation (Hyaluronic acid injection) – effects can vary, but generally last between a few weeks to a few months
- Cortisone Injection (short-term relief of 1-3 weeks)
Surgical Options of Articular Cartilage Preservation:
- Chondroplasty :Involves smoothening uneven edges of cartilage that may ‘catch’ when the joint moves.
- Micro fracture (Abrasion Arthroplasty): Small areas of cartilage loss with exposed bone underneath can be micro-fractured using an instrument that stimulates bleeding into the joint surface, creating new blood supply. This in-turn allows new stem cells from the bone marrow cavity to eventually create a protective form of cartilage preservation.
- Drilling : This is similar to the micro fracture method, whereby multiple holes are made in the joint surface to stimulate a healing response.
- OATs(Osteo-chondralAutograft Transplantation) : A plug of bone, along with its healthy cartilage surface, is transferred from a non-weight bearing part of the knee joint to a defect in the weight bearing surface. When multiple plugs are transferred it is called Mosaicplasty.
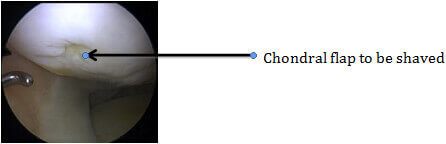

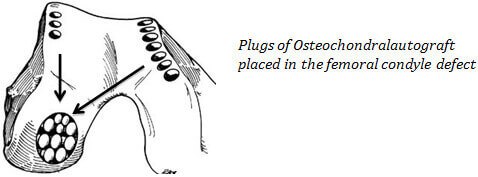
Autologous Chondrocyte Implantation:
These are useful in patients who are younger, where the cartilage defect is more than 2cm2.
This process involves 2 stages:
Stage 1: Cartilage harvesting : Healthy cartilage is tissue removed from the joint surface (non weight-bearing surface) through an arthroscopy. These cartilage cells are then sent to a lab where they are cultured to increase the cell number and make a thin layer of new cartilage.
Stage 2: An open procedure is performed where the defect area is prepared by placing a layer of peri-osteum (bone lining) and sealed at the edges using special fibrin glue. The new cartilage cells are then injected under the lining.
Stem Cell Therapy in Articular Cartilage Damage:
There is currently a huge amount of research and practical work in the topic of cartilage preservation. We now know that mesenchymal stem cells either extracted from bone marrow, fatty tissue (adipose tissue) or even blood can be re-injected into the joint.
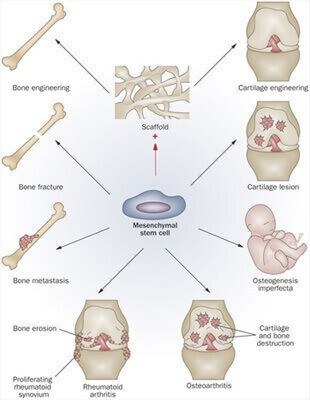
Recent studies have displayed outstanding results where injection of stem cells (with hyaluronic acid) into early to moderate joint wear/cartilage loss, have successfully stimulated new formation over a period of time.
In testing, these results are confirmed by subsequent arthroscopy of the knee joint and biopsy of the cartilage. This is clear when done in conjunction with an orthopaedic procedure like micro-fracture of the joint surface.
Fat derived stem cells have also been injected just on their own into the knee leading to some symptomatic relief of pain and some improvement in function. This may be due to anti-inflammatory properties of the ‘stem cells’ that are injected into the knee rather than actual new cartilage formation.
Platelet Rich Plasma (PRP):
Many professional and recreational athletes claim early return to physical activity with less pain after PRP treatment following musculoskeletal injuries.
What is Platelet Rich Plasma (PRP)?
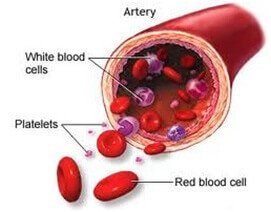
Blood is made up of plasma and important cells (94% red blood cells, white 1-2% blood cells and 5-6% platelets). Platelets are almost 20-25% of the size of red cells. Their main function is to form a clot in order to stop the bleeding process.
How Does PRP Work?
Studies have shown that growth factors and adhesion proteins in PRP can accelerate the healing of injured tissue like tendons, ligaments and joints – acting as a perfect method for cartilage preservation. One of the ways it works is by improving blood supply to damaged tissue therefore speeding up healing.
How is PRP obtained?
By isolating platelets from the blood through a process called Centrifuge. This separates the blood cells from platelets. The result is highly concentrated platelet-rich plasma and growth patterns that are 5-10 times greater than normal.
How is PRP administered?
This can be injected into the damaged tissue, with or without ultrasound guidance depending on the structure that is damaged. Local anaesthetics are usually administered into the area so the patient does not feel any discomfort.
How effective is PRP?
Studies have suggested a 75-85% success rate especially with tendinitis and some joint diseases. If the arthritis is severe, there may be multiple injections of PRP required.
Does PRP cause new cartilage growth in the joints?
There is no evidence that PRP causes new growth of cartilage, but the growth factors and other agents in the platelets have an anti-inflammatory effect that generally relieves pain and improves function, ideal for assisting in cartilage preservation.
Some Common Conditions in which PRP is used:
Ligament and Muscle Injuries:
Acute sporting injuries in professional athletes such as hamstring, knee, ankle and wrist sprains are treatable.
Chronic Tendon injuries:
PRP is known to be very effective in chronic tendon injuries like Achilles tendonitis and also patella tendonitis. It has also been successfully used in the treatment of tennis elbow.
PRP in Surgery:
PRP has been used successfully in conjunction with rotator cuff repairs to enhance healing of the tendon repair. Research is being carried out to discover if ACL repair with PRP provides successful outcomes.
Is PRP a solution to joint replacement?
PRP may be beneficial in sufferers with early to moderate osteoarthritis in joints and loss of cartilage, acting to delay symptoms. But other factors that exacerbate arthritis have to be modified too, such as weight loss, general health & well being and an examination of what activities may be causing damage on joints and blocking cartilage preservation.
In advanced stages, PRP may not be beneficial to some patients, although some studies have shown mild improvements. It will often depend on the individual reactions to treatment from patients. More recent advances in replacement surgery and techniques with technologies mean better outcomes after knee replacements and more effective cartilage preservation when performed by a specialist joint surgeon.










